Why Do the First 40 Days After Birth Matter So Much?

Learn how nutrition, rest, and postpartum rituals support real healing — and why science now backs what tradition has always known.
At a Glance
- The first 6 weeks postpartum are critical for physical healing, hormone regulation, and mental health.
- Traditional “lying-in” practices — warmth, rest, and nourishment — have strong biological foundations.
- Support during this window can shape long-term recovery and maternal well-being.
What Happens in the First 42 Days
Postpartum is more than a recovery period — it’s a recalibration of every major system:
- The uterus contracts from watermelon-sized to pre-pregnancy size
- Hormones like estrogen and progesterone drop sharply, while prolactin and oxytocin rise
- Muscles, ligaments, and nerves that stretched during birth begin to stabilize
- Sleep deprivation and round-the-clock baby care create new stress on mood and immune response
Without recovery support, this period can raise risks of chronic pain, unresolved birth trauma, breastfeeding difficulties, and postpartum depression.
What Traditions Got Right — and Science Now Confirms
In many cultures, the first 30 to 45 days are treated as sacred: a time to rest, nourish, and be cared for. Modern research supports this.
- Warmth and rest: Staying warm and avoiding exertion lowers inflammation and supports
circulation to healing tissues. - Hands-on support: Being cared for (not isolated) reduces maternal stress hormones and boosts
milk production. - Rhythm, not rush: Allowing the body to slow down gives the nervous system space to recalibrate.
This period isn’t about confinement — it’s about recovery without interruption.
What Recovery Needs Beyond the Hospital
Medical care typically ends at discharge or the 6-week OB visit. But recovery continues long after. During this phase, prioritize:
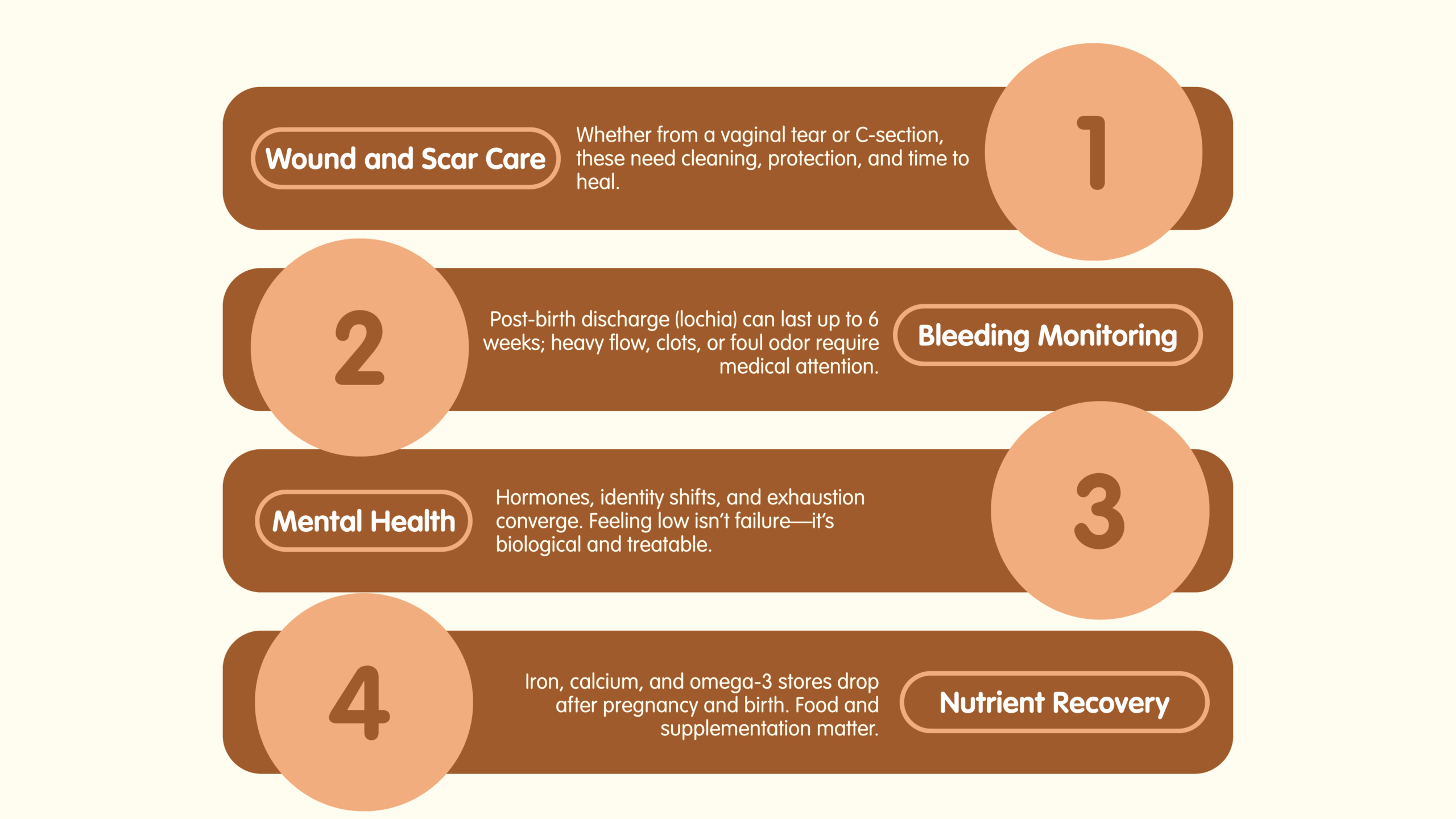
- Wound and scar care: Whether from a vaginal (perineal) tear or cesarean, these need cleaning, protection, and patience.
- Bleeding monitoring: Post-birth discharge (lochia) may last up to 6 weeks — sudden heavy flow, clots, or foul smell need medical attention.
- Mental health: Hormonal shifts, identity changes, and exhaustion converge. Feeling low isn’t failure — it may be biology, and it’s treatable.
- Nutrient recovery: Iron, calcium, and omega-3 stores drop after pregnancy and birth. Food and supplementation matter.
What to Do Next: Guidance for Pregnant Moms
- Set boundaries early — ask your support system to bring food, hold baby, or help clean so you can recover.
- Prioritize restorative meals: warm, protein-rich, iron-boosting dishes.
- Discuss with your OB if you feel prolonged sadness, can’t rest, or notice heavy bleeding or
infection symptoms.
Note:
This article was medically reviewed and written in collaboration with doctors and medical professionals committed to providing pediatric health education.
References:
World Health Organization (WHO) – Maternal and Perinatal Health
American College of Obstetricians and Gynecologists (ACOG)
Centers for Disease Control and Prevention (CDC – U.S.) – Pregnancy

Marie Victoria S. Cruz-Javier, MD, FPOGS, FPSGE
Obstetrics and Gynecology Minimally Invasive Gynecologic Surgery and Robotic Surgery Aesthetic Gynecology
Disclaimer:
The information in this article is intended for educational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician, pediatrician, or qualified healthcare provider with any questions you may have regarding a medical condition or health objectives.
