Are These Pregnancy Symptoms Normal or a Sign to Inform My OB as soon as possible?
Get trimester-by-trimester clarity on what to expect, what to monitor, and when something needs a closer look.

At a Glance
- Many symptoms are common but can feel alarming — tracking when they happen matters.
- Bleeding, severe pain, and unusual discharge should never be ignored.
- When in doubt, inform your doctor. It’s always safer to get checked early.
First Trimester: New, Strange, and Often Normal
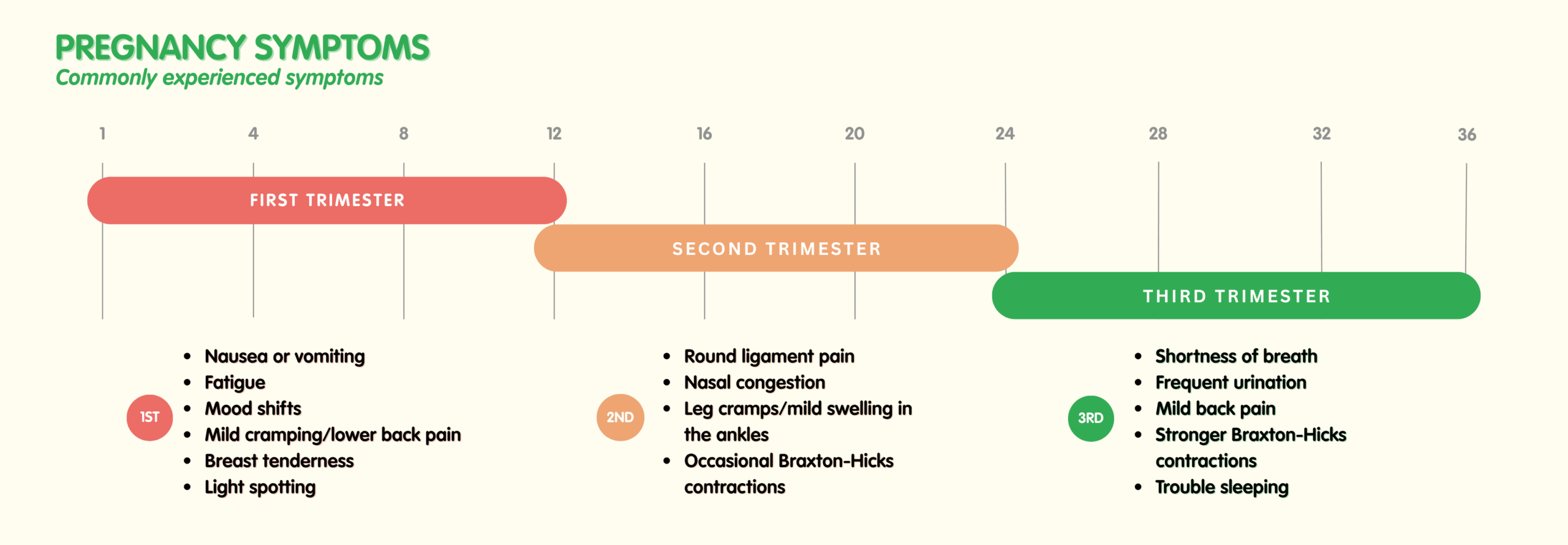
Your body is adjusting fast to hormonal changes. Common symptoms include:
- Nausea or vomiting
- Fatigue
- Mood shifts
- Mild cramping or lower back pain
- Breast tenderness
- Dizziness
Inform your OB immediately, if you experience:
- Heavy bleeding
- Bright red bleeding
- Fainting or severe headache
- Severe abdominal pain, especially if one-sided
- Fever over 38°C
- Painful urination or cloudy urine
Second Trimester: More Stable, Still Watchful
Many women feel better now — nausea eases, energy returns, and appetite improves. Common symptoms include:
-
Round ligament pain (brief sharp groin pain with movement)
-
Leg cramps or mild swelling in the ankles
-
Occasional Braxton-Hicks contractions
Inform your OB if you notice:
- Persistent headaches or vision changes
- Severe pain that doesn’t ease with rest
- Leaking fluid or watery discharge
These may be early signs of preeclampsia, infection, or preterm labor.
Third Trimester: Baby Is Growing, So Are the Demands
Normal symptoms now include:
- Shortness of breath
- Frequent urination
- Mild back pain
- Stronger Braxton-Hicks contractions
- Trouble sleeping
However, call your OB if you experience:
- Decreased fetal movement (fewer than 10 kicks in 2 hours)
- Sudden severe abdominal pain
- Vaginal bleeding
- Persistent vomiting
- Severe swelling or headache
- Contractions before 37 weeks
What to Do Next: Guidance for Pregnant Moms
- Keep a symptom tracker or note app to monitor patterns over time, and discuss with your OB
during check-up. - If symptoms escalate quickly (bleeding, severe pain, fever), go directly to the ER or your delivery
hospital.
Note:
This article was medically reviewed and written in collaboration with doctors and medical professionals committed to providing pediatric health education.
References:
World Health Organization (WHO) – Maternal and Perinatal Health
American College of Obstetricians and Gynecologists (ACOG)
Centers for Disease Control and Prevention (CDC – U.S.) – Pregnancy

Marie Victoria S. Cruz-Javier, MD, FPOGS, FPSGE
Obstetrics and Gynecology Minimally Invasive Gynecologic Surgery and Robotic Surgery Aesthetic Gynecology
Disclaimer:
The information in this article is intended for educational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician, pediatrician, or qualified healthcare provider with any questions you may have regarding a medical condition or health objectives.
