What Are My Pain Relief Options for Labor?

Explore natural techniques, epidurals, and new tools to create a birth plan that matches your comfort and your goals.
At a Glance
- Labor pain can be managed in many safe ways — from breathing to medication.
- Choosing ahead helps reduce fear and makes your birth plan more focused.
- What works best is different for every mother — your comfort is valid and personal.
Understand the Pain, Plan for the Choice
Labor pain comes from strong uterine contractions, cervical changes, and pressure on pelvic nerves. But pain is also emotional: fear, tension, and exhaustion all amplify it. That’s why pain management needs to address both the body and the mind.
You don’t need to decide everything in advance — but knowing your options lets you respond with clarity, not panic.
Pain relief choices fall into two broad types: non-medicated (natural techniques) and medicated (regional or systemic anesthesia). Many women combine both during labor.
Non-Medicated Pain Relief Techniques
These methods work best when started early, with support and preparation.
- Breathing and relaxation techniques — paced breathing calms the nervous system and reduces muscle tension.
- Movement and positioning — swaying, walking, or kneeling can ease pressure and help baby descend.
- Warm compress or shower — heat therapy soothes muscles and may reduce the need for medication.
- Massage and counterpressure — especially during back labor; best with a trained birth partner or doula.
- Water immersion — some hospitals offer labor tubs (not to be confused with water birth).
- TENS machine — delivers mild electrical pulses to interrupt pain signals. Ask your OB if available.
These work well for early and active labor but may not fully relieve intense pain in transition or pushing.
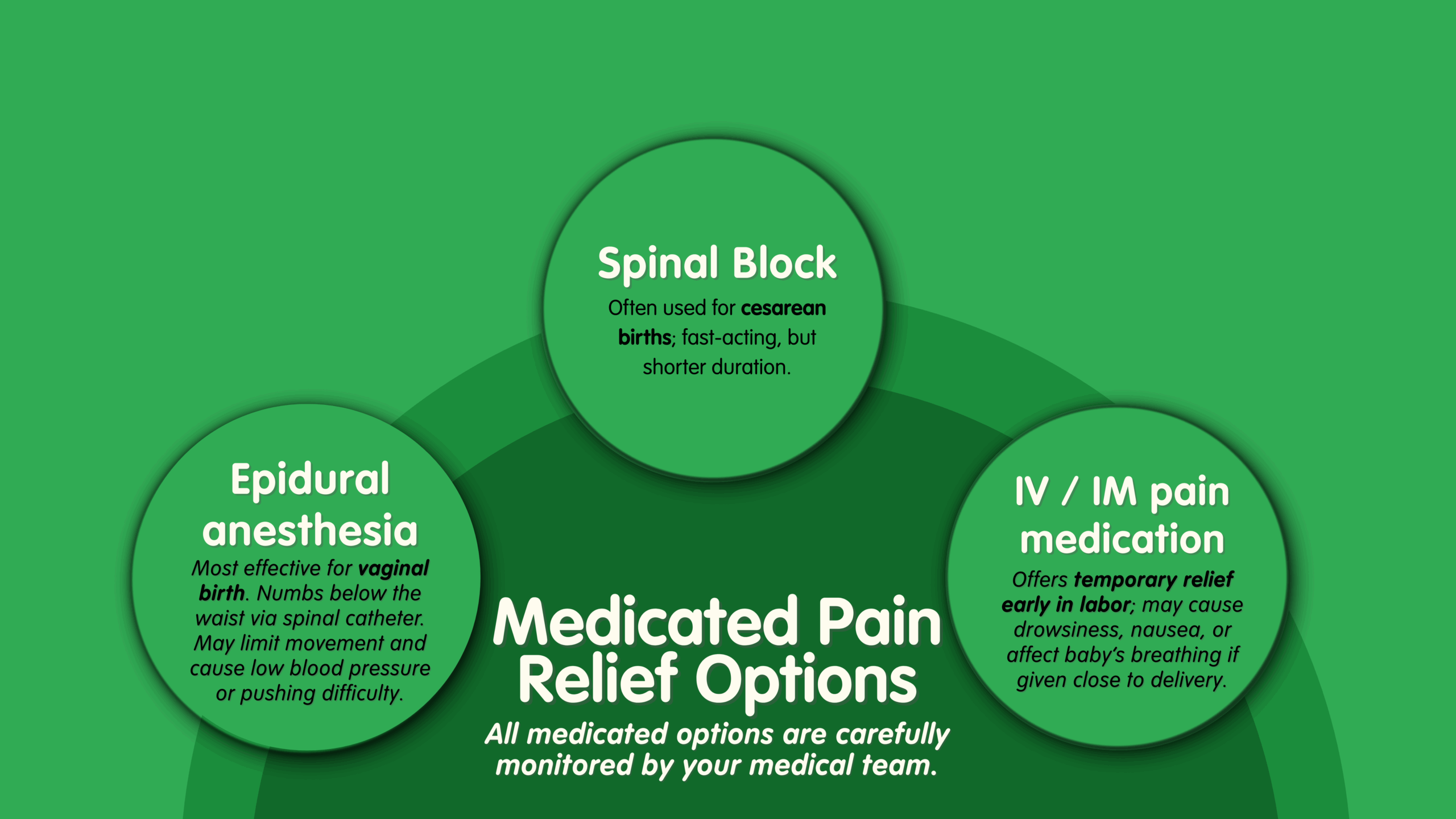
Medicated Pain Relief Options
- Epidural anesthesia
- Most effective pain relief for vaginal birth.
- A catheter delivers medication near the spinal cord, numbing sensation below the waist.
- Takes 10–15 minutes to work; may reduce ability to move freely.
- Side effects: drop in blood pressure, difficulty pushing in some cases, may need assisted delivery.
- Spinal block
- Often used for cesarean births; fast-acting, but shorter duration.
- IV or IM pain medication (opioids)
- Provides temporary relief, often in early labor.
- Can cause drowsiness or nausea; may affect baby’s breathing if given too close to delivery.
All medicated options are closely monitored and adjusted by your medical team.
What to Do Next: Guidance for Pregnant Moms
- Discuss with your OB which options your hospital supports — not all offer labor tubs or TENS.
- Include both medicated and non-medicated preferences in your birth plan — stay flexible.
- Let your support person know how to advocate for your comfort if you’re unable to speak much during active labor.
Note:
This article was medically reviewed and written in collaboration with doctors and medical professionals committed to providing pediatric health education.
References:
World Health Organization (WHO) – Maternal and Perinatal Health
American College of Obstetricians and Gynecologists (ACOG)
Centers for Disease Control and Prevention (CDC – U.S.) – Pregnancy

Marie Victoria S. Cruz-Javier, MD, FPOGS, FPSGE
Obstetrics and Gynecology Minimally Invasive Gynecologic Surgery and Robotic Surgery Aesthetic Gynecology
Disclaimer:
The information in this article is intended for educational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician, pediatrician, or qualified healthcare provider with any questions you may have regarding a medical condition or health objectives.
